Bridging the Gap: How Innovation and Philanthropy Can Redefine Maternal and Child Health in India

India Health Fund (IHF), since its inception has been a catalytic force in developing and validating technologies and innovations that accelerate the elimination of infectious diseases such as Tuberculosis and Malaria, alongside other critical public health challenges. IHF has long recognised the transformative potential of health technology in driving ambitious, measurable improvements in health outcomes. Building on this proven platform, which has expanded healthcare access through affordable diagnostics and digital solutions at the primary care level, IHF is now poised to extend its impact to maternal and child health (MCH) across India.
MCH Scenario in India
India has achieved remarkable progress in Maternal and Child Health (MCH) outcomes, with sustained declines in the Maternal Mortality Ratio (MMR) and Neonatal Mortality Rate (NMR) that have consistently outpaced global and regional averages. This progress reflects strong political and administrative will, robust governance frameworks, expanded health infrastructure, and demand-driven interventions, notably the Janani Shishu Suraksha Karyakram (JSSK) and Janani Suraksha Yojana (JSY) which have significantly improved MCH service utilisation and institutional delivery rates.
India has achieved remarkable progress in Maternal and Child Health (MCH) outcomes, with sustained declines in the Maternal Mortality Ratio (MMR) and Neonatal Mortality Rate (NMR) that have consistently outpaced global and regional averages. This progress reflects strong political and administrative will, robust governance frameworks, expanded health infrastructure, and demand-driven interventions, notably the Janani Shishu Suraksha Karyakram (JSSK) and Janani Suraksha Yojana (JSY) which have significantly improved MCH service utilisation and institutional delivery rates.
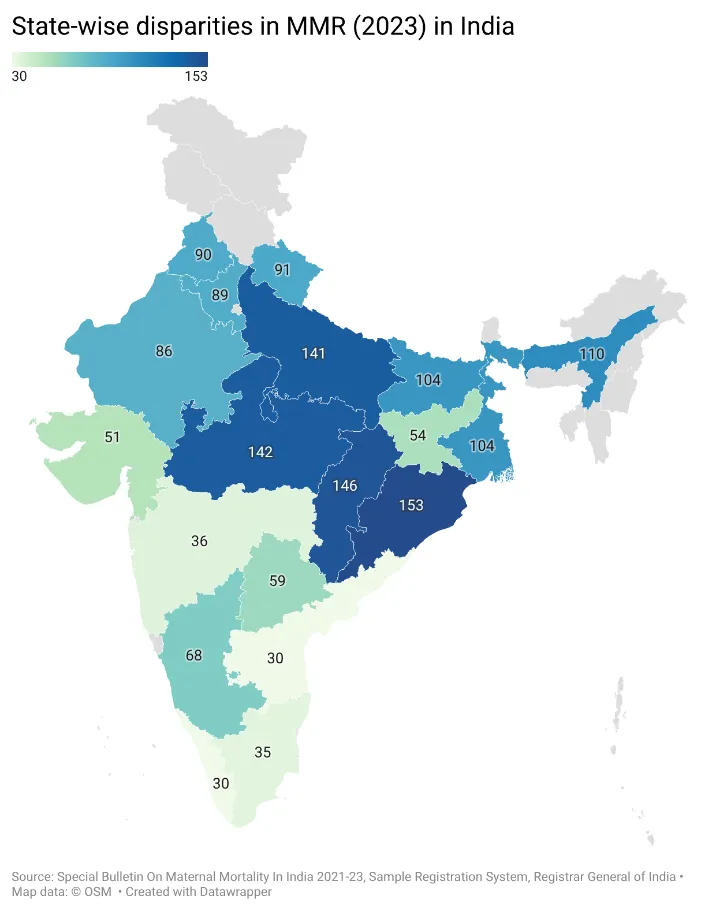
Causes of Maternal and Neonatal Mortality
The leading causes of maternal deaths are obstetric haemorrhage, followed by hypertensive disorders and sepsis along with continued burden of indirect causes like anaemia, heart disease, and other infectious diseases. Notably, haemorrhage accounts for a disproportionately higher share of deaths in Bihar, Uttar Pradesh, and Uttarakhand, while hypertensive disorders are more prevalent among maternal deaths in Maharashtra, Tamil Nadu, and Kerala, reflecting the broader epidemiological transition from communicable to non-communicable disease burden underway in these states.
Furthermore, severe anaemia combined with delayed recognition and management of intrapartum complications may exacerbate postpartum haemorrhage underscoring the importance for a strong Antenatal Care (ANC) coverage. Women from lower wealth quintiles bear a disproportionate burden of anaemia and face the greatest impact from delays across the continuum of care. On the neonatal side, prematurity and low birth weight, birth asphyxia, and birth trauma remain leading causes of neonatal mortality, each closely interconnected with maternal morbidities such as hypertension and anaemia.
Systemic Factors affecting Maternal and Neonatal Mortality
Systemic gaps including delays in seeking timely care, limited access to emergency maternal services, and inconsistent quality of service delivery remain key drivers of poor maternal and child health outcomes. These gaps translate into critical delays across the caregiving continuum, with serious consequences for both mother and newborn. While conditional cash transfer programmes such as JSY have successfully driven institutional deliveries, the quality of obstetric care remains a significant and unresolved contributor to maternal mortality. Even though, ANC 4+ visit coverage has improved to 58%, the quality and effective coverage of ANC among women remains sub-optimal underscoring that mere coverage does not guarantee meaningful care. India’s health system has made meaningful strides in access, successfully driving demand for MCH care. However, quality dimensions including safety, timeliness, effectiveness, person-centred care, and the efficient, equitable use of resources remain a persistent challenge, unless technology and innovation is leveraged.
Existing Technology Landscape for Maternal and Child Health
Technology has become an increasingly visible part of MCH programmes in low and low-middle income countries. In India, this shift has taken place around broader efforts to expand antenatal care, improve institutional deliveries and strengthen frontline health workforce with specific use-cases for digital health platforms. Timely management of maternal and foetal complications across all stages of pregnancy can be significantly strengthened through Point-of-Care (PoC) diagnostics for early screening and diagnosis of maternal morbidities, and AI-based digital solutions that enable continuous monitoring of maternal and foetal vital parameters, facilitating risk prediction, prompt escalation, and timely referral.
Despite the advent of PoC screening tools for anaemia, infections, miniaturised AI-based devices for pregnancy monitoring and mHealth tools to register pregnancies, track ANC and follow up with beneficiaries, its adoption in routine public health system remain largely limited. While these technologies have demonstrated evidence of improving service coverage, their impact on health outcomes is contingent on the strength of care continuum and broader delivery systems. These solutions operate in silos, with low interoperability with public health data systems and complex interfaces that affect usability among frontline workers. As a result, availability of frontier technologies does not always translate into better health outcomes for the population.
Sustained investment in a more system-aligned approach to innovation is essential to translating access gains into genuinely improved maternal and child health outcomes by building a health system that is not merely accessible, but truly high-quality.
IHF’s Innovation Partnership
Given the critical importance of improving maternal and child health, quality of care and access to ANC to reduce newborn and maternal mortality; IHF has now ventured into an innovation partnership under the “Empowering Mothers with Birth Readiness, Agency, and Care” (EMBRACE) programme. EMBRACE offers a compelling model for how partnerships can transform maternal and child health outcomes in low- and middle-income countries. At its core is a powerful collaboration between a philanthropic anchor focussed on maternal and child health with extensive presence in India and Africa, where IHF will now apply its proven model of supporting innovation development for public health challenges to identify potential approaches to develop affordable, minimally and non-invasive diagnostics and pregnancy management tools for use in primary care in low resource settings.
Over the next three years, IHF will build a structured pipeline of solutions in a set of maternal focused priority areas (Figure), supporting mid to late-stage solutions through product development, clinical and operational validation, and evidence generation; with
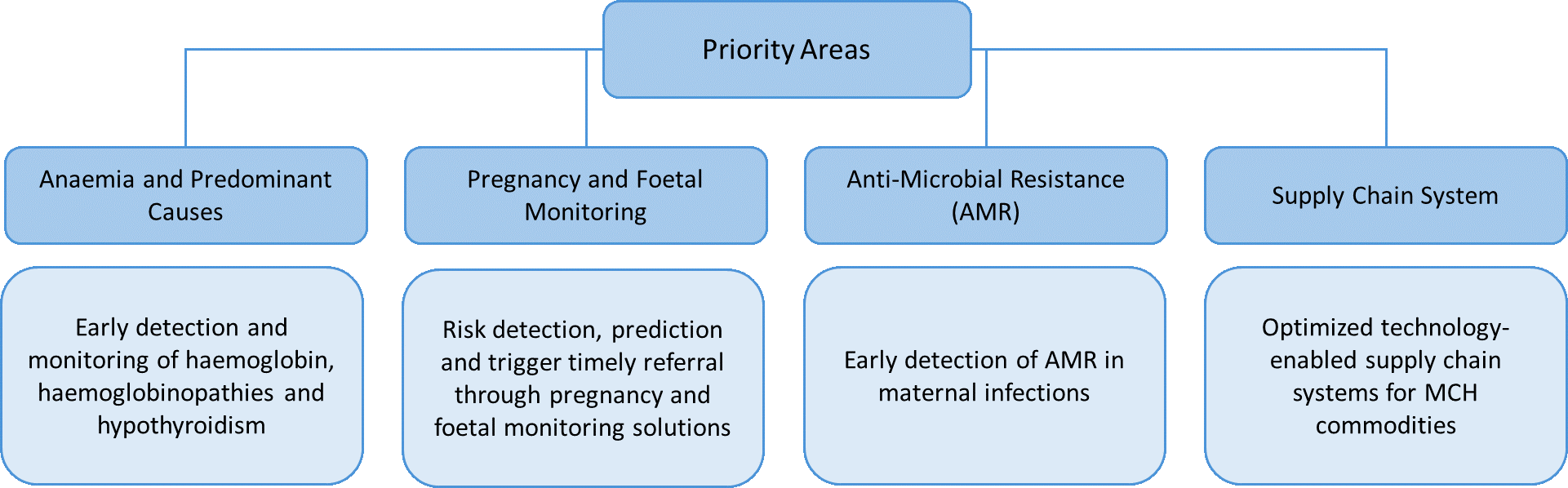
deployment through local implementation partners who bring critical contextual knowledge and ensure last-mile delivery. The areas of focus will be expanded or modified as the initiative develops and can also be adapted to meet the specific innovation requirements of partners. This approach will bridge the evidence to adoption gap for science-based innovations in maternal health by embedding innovations into service delivery models, supply chains and clinical practice.
Catalytic Role of Philanthropy in Maternal and Child Health
With 21% decline in global development assistance for health and further forecasted decline in the coming years, regional and domestic philanthropies need to collaborate position itself as a lever to mobilize private or multilateral finance and support capacity building in civil society and local institutions to sustain and accelerate the health gains achieved in India over the last decades. Philanthropy provides catalytic capital and risk appetite, multilaterals bring scale and systems alignment, and local partners translate innovation into real-world impact. As a catalytic actor, philanthropy can help reduce risk in early-stage innovation and support solutions that may not yet attract commercial investment. Therefore, IHF is exploring partnerships to build a coalition that supports the development, validation and deployment of maternal and child health innovations. These solutions can then be scaled in low and low-middle income countries through these programme partners and collaborating foundations.
India stands at a pivotal moment in its maternal and child health journey where progress in access must now be complemented by high-quality care. The path forward demands more than incremental change; it calls for bold, system-aligned innovation that is deeply embedded in care delivery and responsive to the realities of the underserved populations. India can transform its health system into one that not only saves lives but ensures that every mother and child thrives. The opportunity is not just to meet MCH targets, but to redefine what sustainably financed, equitable, high-quality, innovation-led maternal and child healthcare looks like for the country.
Conclusion:
Samyak is a health initiative housed within Collective Good Foundation (CGF), committed to improving the quality of life of India’s urban citizens by bridging existing health inequities. Samyak – CGF is a knowledge partner to the Government of Uttar Pradesh (GoUP), providing support to improve health and nutrition outcomes in 100 small, transitioning cities through the UP Aspirational Cities Program (UP-ACP). UP – ACP is a flagship program of the GoUP that aims to improve municipal service delivery, create economic opportunities and improve the quality of life of all citizens. The program identifies social infrastructure (health and education) as a key pillar for urban transformation, indicating GoUP’s commitment to improve urban health outcomes and recognition of the potential role of ULBs in this process.
The study was conducted to understand and examine the health status and challenges in these cities. The findings from the study have been shared with the Urban Development Department, Government of UP, the anchor for the UP–ACP program. Samyak is currently working with the Government (including the state health department) and other development partners in UP to collectively address these challenges through a system-led approach.
Authors:

Dr. Aatmika Nair, Manager – Portfolio, India Health Fund

Samrudhi Khanna , Sr. Associate, India Health Fund
